

Dell and Northwestern Medicine Collaborate on Next Generation Healthcare Multimodal LLMs
Thu, 15 Feb 2024 15:56:13 -0000
|Read Time: 0 minutes
Generative multimodal large language models, or mLLMs, have shown remarkable new capabilities across a variety of domains, ranging from still images to video to waveforms to language and more. However, the impact of healthcare-targeted mLLM applications remains untried, due in large part to the increased risks and heightened regulation encountered in the patient care setting. A collaboration between Dell Technologies and Northwestern Medicine aims to pave the way for the development and integration of next-generation healthcare-oriented mLLMs into hospital workflows via a strategic partnership anchored in technical and practical expertise at the intersection of healthcare and technology.
One practical application of mLLMs is highlighted in a recent open-source publication from the Research and Development team at Northwestern Medicine which describes the development and evaluation of an mLLM for the interpretation of chest x-rays. These interpretations were judged by emergency physicians to be as accurate and relevant in the emergency setting as interpretations by on-site radiologists, even surpassing teleradiologist interpretations. Clinical implementation of such a model could broaden access to care while aiding physician decision-making. This peer-reviewed study – the first to clinically evaluate a generative mLLM for chest x-ray interpretation – is just one example of the numerous opportunities for meaningful impact by healthcare-tailored mLLMs.
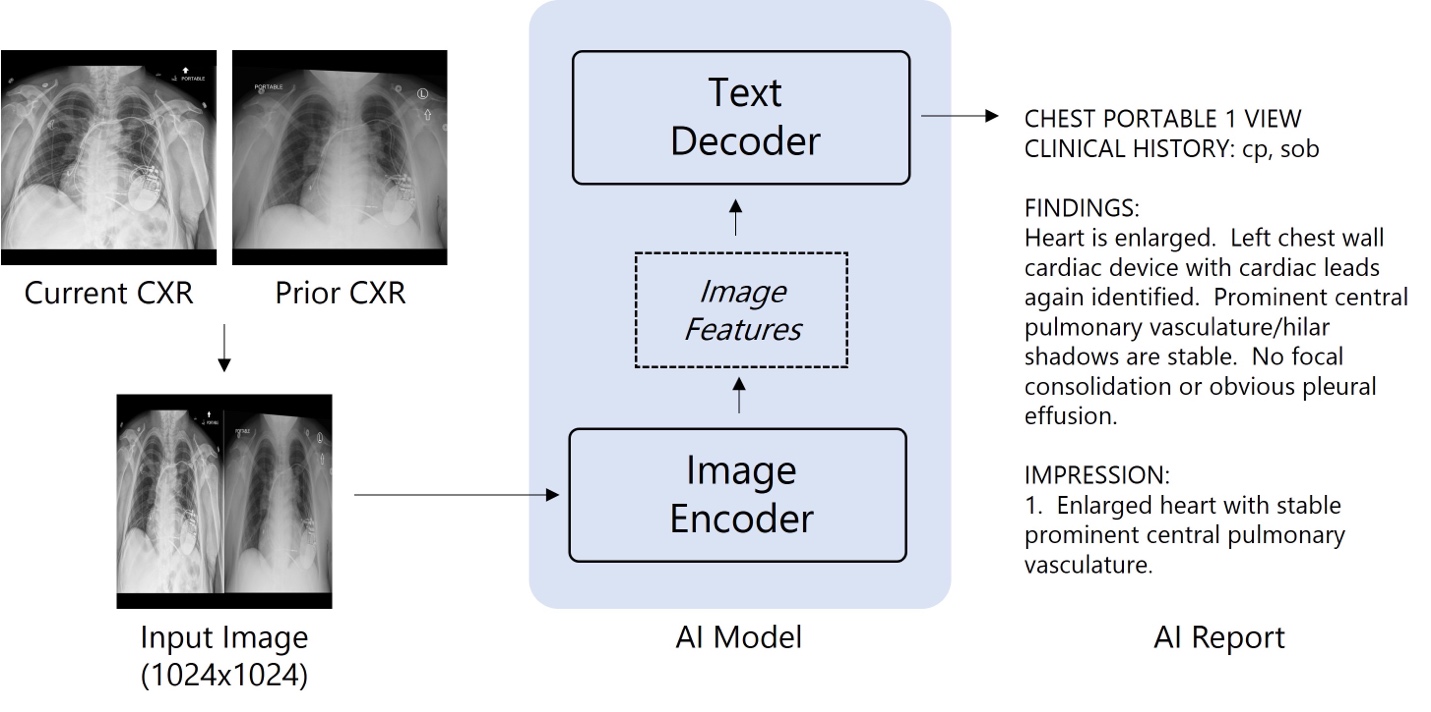 Figure 1. Model architecture for chest x-ray interpretation
Figure 1. Model architecture for chest x-ray interpretation
As illustrated in Figure 1, the model is a vision encoder-decoder model, using pretrained ViT-base and RoBERTa-base as the image encoder and text decoder respectively. In total, over 1 million images and radiology reports were used to train this model using one node with 8 GPUs over three weeks. Expanding the scope of such models, such as to other image modalities like computed tomography and magnetic resonance imaging, requires much greater hardware capabilities to efficiently train at scale.
Notably, this model was trained using only 8 graphics processing units (GPUs) in three weeks. As the broader body of LLM research has shown, there is great promise in scaling up such methods, incorporating more data and larger models to create more powerful solutions. Hospital systems generate vast amounts of data spanning numerous modalities, such as numeric lab values, clinical images and videos, waveforms, and free text clinical notes. A key goal of the collaboration between Dell Technologies and Northwestern Medicine is to expand on this work and scale the capabilities of healthcare systems to use their own data to solve clinical problems and blend cutting edge data-centric platforms with clinical expertise, all targeted toward improving the patient and practitioner experience.
HIPAA Compliant HPC
To bring this vision to fruition, it is necessary to build out capable healthcare-tailored high-performance computing (HPC) clusters in which multiple nodes with varying levels of compute, memory, and storage resources are made available to users to run tasks in parallel and at scale. This enables centralized management of resources with the flexibility to provision resources to jobs ranging from single-node experiments to massively distributed model training. The typical HPC cluster structure is illustrated in Figure 2. Users can connect to a login node via virtual private network (VPN) or secure shell (SSH). These nodes provide access to requested compute resources within the internal HPC cluster network as well as job scheduling software, such as slurm, to coordinate job submission and distribution. Computing nodes are interconnected with varying levels of provisioned access available, ranging from one GPU on a multi-GPU node to dozens of multi-GPU nodes. A shared parallel filesystem is used to access the data storage.
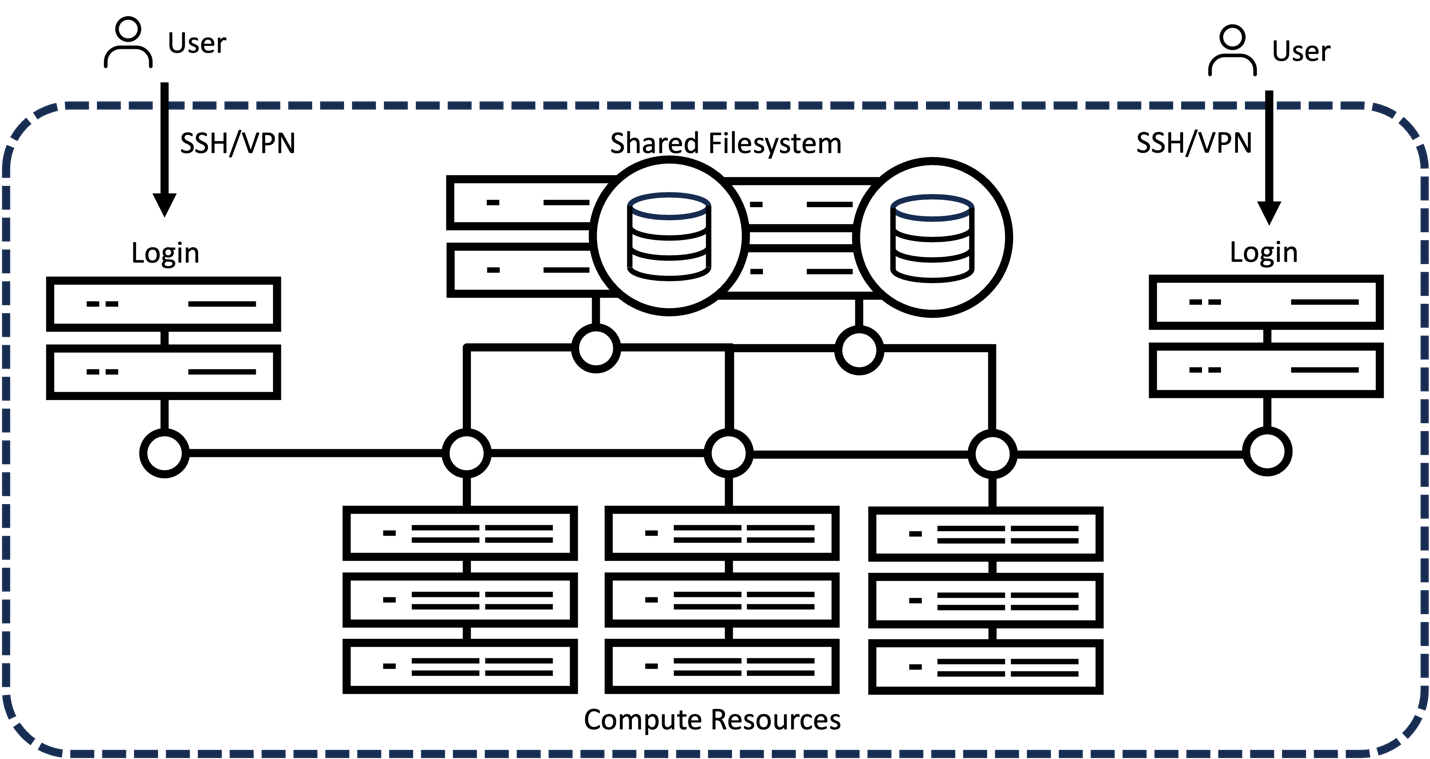 Figure 2. Typical HPC cluster setup
Figure 2. Typical HPC cluster setup
However, a special consideration within ecosystems handling hospital data is protected health information, or PHI. The Health Insurance Portability and Accountability Act, or HIPAA, mandates a basic level of security to ensure that PHI is adequately protected, ensuring patient privacy around sensitive health data. Thus, HIPAA-compliant healthcare HPC must account for heightened security and segregation of PHI. But what exactly does it mean to be HIPAA compliant? The following will describe some key components necessary to ensure HIPAA compliance and protection of sensitive patient data throughout all aspects of hospital-based collaborations. Though HIPAA compliance may seem challenging, we break down these requirements into two key facets: the data silo and data stewardship, as shown in Figure 3.
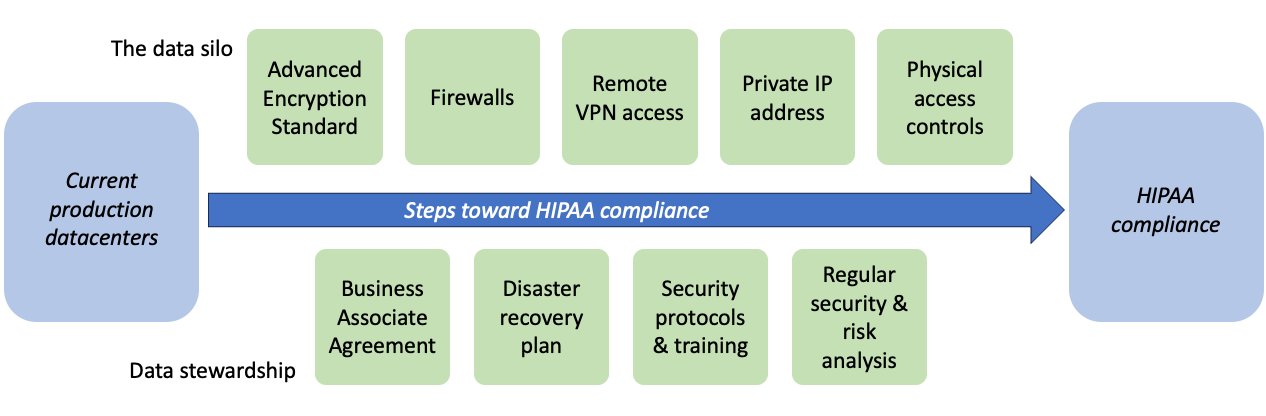 Figure 3. The key facets needed to ensure HIPAA compliance in datacenters housing healthcare data
Figure 3. The key facets needed to ensure HIPAA compliance in datacenters housing healthcare data
Firstly, the data silo must ensure that access is provisioned in a secure and controllable fashion. Data must be encrypted in accordance with the Advanced Encryption Standard (AES), such as by AES-256 which utilizes a 256-bit key. Adequate firewalls, a private IP address, and access via remote VPN are further required to ensure that PHI remains accessible only to authorized parties and in a secure fashion. Finally, physical access controls ensure credentialed access and surveillance within the datacenter itself.
Secondly, data stewardship practices must be in place to ensure that practices remain up to date and aligned with institutional goals. A business associate agreement (BAA) describes the responsibilities of each party with regards to protection of PHI in a legally binding fashion and is necessary if business associate operations require PHI access. Security protocols, along with a disaster recovery plan, should be outlined to ensure protection of PHI in all scenarios. Finally, regular security and risk analyses should be performed to maintain compliance with applicable standards and identify areas of improvement.
While many datacenters have implemented measures to ensure compliance with regulations like HIPAA, the greatest challenge remains providing on-demand separation between general workloads and HIPAA-compliant workloads within the same infrastructure. To address this issue, Dell Technologies is working in collaboration with Northwestern Medicine on a new approach that utilizes flexible, controlled provisioning to enable on-demand HIPAA compliance within existing HPC clusters, as shown in Figure 4. This HPC setup, once deployed, would automatically provide network separation and the reconfiguration of compute and data storage resources, ensuring they are isolated from the general allocation.
This newly HIPAA-compliant portion of the cluster can be accessed only by credentialed users via VPN using dedicated login nodes which provide separate job scheduling and filesystem access, enabling access to AI-ready compute resources without disrupting general workloads. When no longer needed, automatic cluster reconfiguration occurs, returning resources to the general allocation until new HIPAA-compliant workloads are needed.
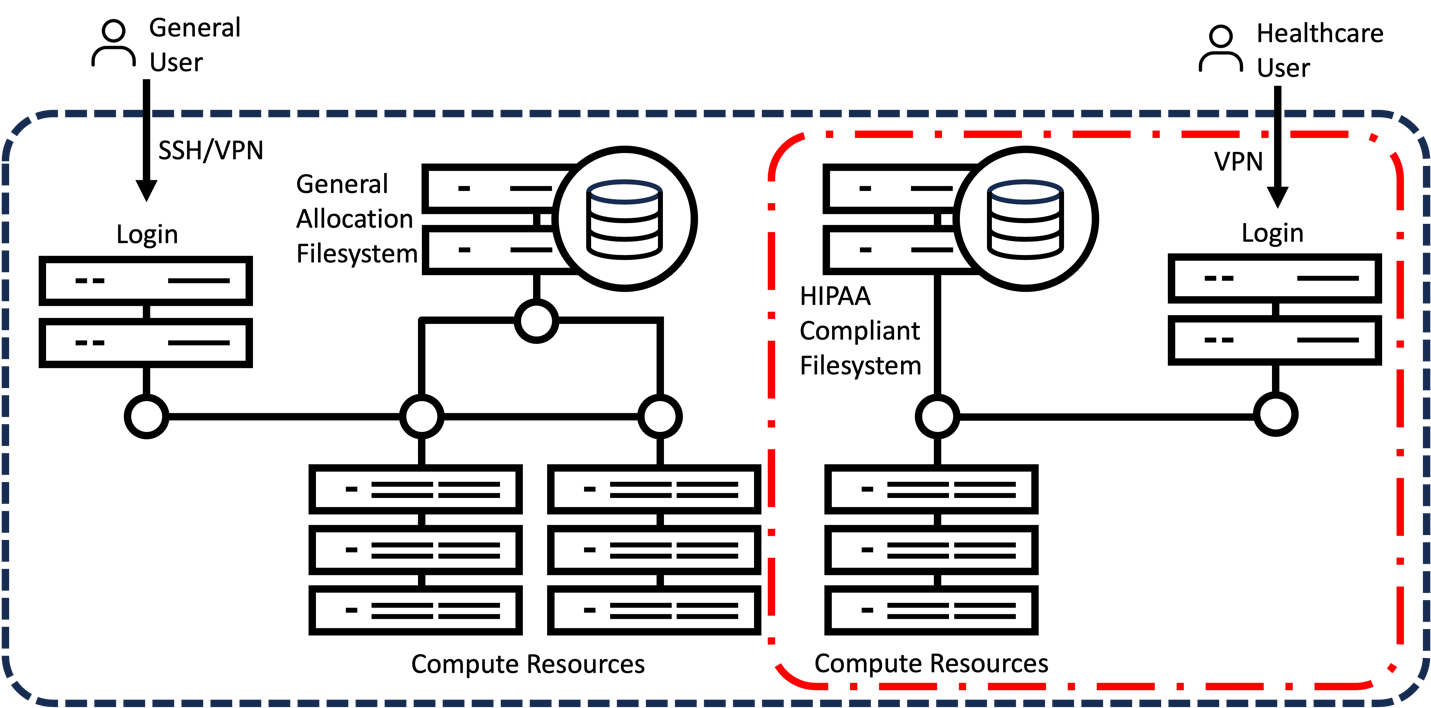 Figure 4. Next-generation HIPAA-compliant HPC cluster, which builds on the typical setup presented in Figure 1
Figure 4. Next-generation HIPAA-compliant HPC cluster, which builds on the typical setup presented in Figure 1
Our expertise in compute infrastructure for artificial intelligence (AI) initiatives extends to developing datacenters and datacenter infrastructure with the proper security and controls in place that a health system can leverage as part of their efforts in achieving HIPAA compliance.
This integrated model of HIPAA-compliant compute for healthcare is aimed at democratizing the benefits of the artificial intelligence revolution, enabling healthcare institutions to employ these new technologies and provide better, more efficient care for all.
Resources
Generative Artificial Intelligence for Chest Radiograph Interpretation in the Emergency Department: https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2810195
Author:
Jonathan Huang, MD/PhD Candidate, Research & Development, Northwestern Medicine
Matthew Wittbrodt, Solutions Architect, Research & Development, Northwestern Medicine
Alex Heller, Director, Research & Development, Northwestern Medicine
Mozziyar Etemadi, Clinical Director, Advanced Technologies, Northwestern Medicine
Bhavesh Patel, Sr. Distinguished Engineer, Dell Technologies
Bala Chandrasekaran, Technical Staff, Dell Technologies
Frank Han, Senior Principal Engineer, Dell Technologies
Steven Barrow, Enterprise Account Executive



